The Nuclear Test Veterans Model

Jean-François GRENOT (GrenotClinvest) researcher for OBSIVEN France introduces his area of interest for his next research project. – Project manager of medical studies for OBSIVEN France. In memory of Jean-Louis FERRER (Vice President of AVEN).
Introduction
While the presence of military personnel at nuclear tests has subsequently resulted in many delayed health effects that are difficult to prove, it is even more difficult to demonstrate the cardiac pathologies associated with exposure to ionizing radiation.1
In French veterans, a significant increase in heart disease was found (Valatx Survey) compared to the normal population at the time of the survey.
In France and other nuclear-capable countries, Heart disease is not directly related to the impact of radiation on their nuclear test veterans, only conditions like tumours and cancers are officially recognised.
However, detonations of nuclear devices are not the only source of radiation that can affect the human body, incidents of radiation leakage from nuclear power plants, medical imaging and radiation treatments all appear to impact on the heart. This has been documented in publications.
What future and what consequences could we derive from research and observations made in medicine for nuclear veterans?
The heart
The heart is a muscle that can distribute blood flow throughout the human body. It has a role of pump that is to say it sucks the blood and expels it. Thus allowing the supply of nutrients and oxygen in the form of oxyhemoglobin to the cells, and also the return of “waste” resulting from the respiratory process.
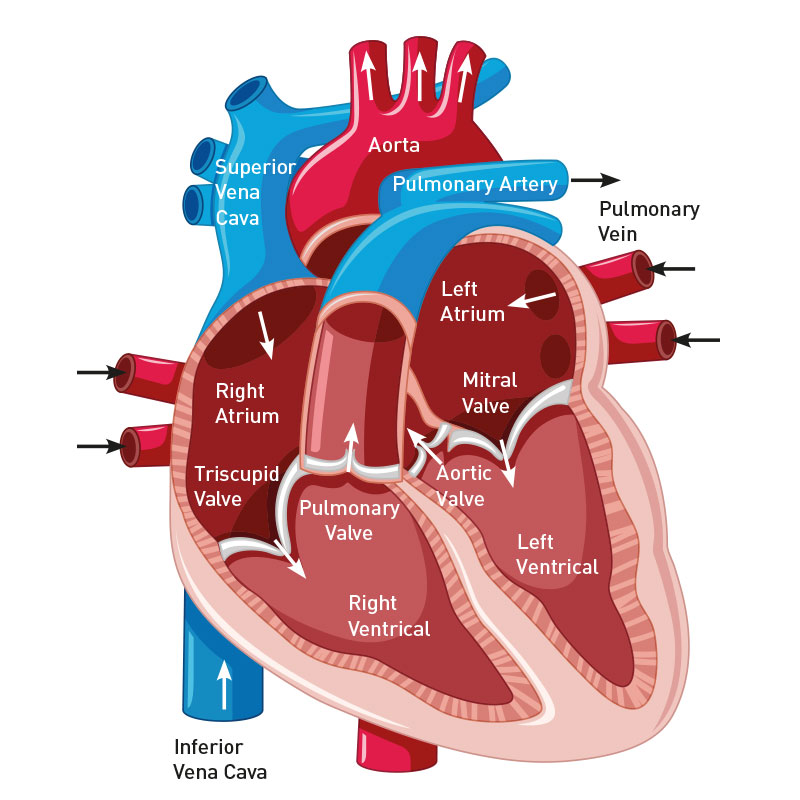
Fig.1 Diagram of the heart
Cardiac dysfunction is called heart disease. The heart is made up of 4 cavities (right atrium, right ventricle, left atrium and left ventricle), it is obvious that a lesion on the cells of this muscle (cardiomyocytes), will have various consequences according to the location of the injured cells. In particular, the ischemic consequences (lack of oxygen supply) on the organs and on the cardiac muscle (myocardium) itself causing cell death (necrosis), which is called myocardial infarction.
Low doses of radiation used in human medicine
Medical imaging
Radiation has been used since the end of the 19th century to pass through the body in order to establish an image allowing an examination of the internal organs. These radiations are invisible and interact with the tissues to create an image.
X-rays used in classical medical radiology are stopped by dense structures (bones, lungs …). Thus, they transmit images of the contour of the non-traversed components.
The higher the energy (dose) of these radio waves, the more penetrative power they have, increasing the ionization of the cells through which they pass.2

Fig.2 Radiation and medical imaging
Repeated low-dose ionization such as that used in medical radiology (scintigraphy and tomography) eventually creates an intrinsic modification of the DNA (genome) of the cells penetrated with repairable or non-repairable damage depending on the genes affected by it.
Fortunately, there are repair genes or ‘killers of the genomic lesion’. The fact is that repair or apoptosis (cell death) is only possible if the genes involved in these two actions are not impacted themselves by the ionizing radiation.
Radiotherapy
In the context of cancer treatment, radiation is used under strictly controlled conditions, for example, targetting tumours that would be difficult to reach by conventional surgery. Thus are used for the purpose of tumour removal with or without chemotherapy.
As we have already explained, the tissues crossed are more likely to be damaged. It is not uncommon to find skin lesions (inflammation of the skin) to radiodermatitis (inflammation under the skin associated with radiation) during the course of treatment.
So, it would be logical in the context of chest radiotherapy targeting inaccuracies or too high strength, to be able to observe the appearance of cardiac lesions. This cardiotoxic character of radiotherapy has been observed, recently, in patients with cancer and treated for it.3 Bringing into question their quality and expectancy of life.
This phenomenon of cardiac lesions was described in 2003, warning about the consequences of radiation on the pericardium (cardiac envelope) and the myocardium in patients who underwent radiotherapy after mastectomy (removal of the breast).4
The mechanisms of damage to myocardial cells by high energy radiation exist but are poorly documented at present.5
Animal experimentation
RNA (ribonucleic acid) has a function of transcription of DNA and also micro-repair. Hence the name micro-RNA in the context of gene repair. The production of these micro-RNAs increase along with increases to lesions of the genes (the more work to do, the more workers are produced).
Very recently, it has been determined in mice subjected to low dose radiation repeated over a period of four months, that increased levels of micro-RNA were detected in the Liver and Testicles but mostly in the heart. This would demonstrate that through this activity of regulating the genome in these mammals, repeated low-dose radiation will cause damage.6
Genetic mutations of myocardial cells sometimes leading to major malformations in mice have been described. The younger the individual, the more it appears that the abnormalities are important. Thus, during embryogenesis, while the heart is forming, abnormal interactions between the different compartments have been observed after irradiations of small repeated doses.7 It is then possible to talk about congenital anomalies related to low doses.
Discussion
The animal model, and in particular the mouse, is very often used to show cardiac alterations related to radiation.
In addition to this, the diagnostic and therapeutic tools used in medicine have largely demonstrated epidemiologically, an increase in the morbidity of treated individuals and an alteration of their quality of life. Although this is not the subject of this article, we could in some cases evaluate the benefit/risk balance of radiation treatments by reconsidering the age and general condition of patients.
Originally, veterans of nuclear testing are not patients. They have a high probability of becoming so many years later because they have the same negative consequences as patients treated for cancer at the outset.
They suffer a stochastic effect (over the long term) that has been more or less recognized depending on the nation that conducted the nuclear tests. But in almost all cases, the recognized conditions of exposure are limited to tumours and cancers. No heart disease appears on the official recognition and compensation lists.
Conclusion
According to Jean-Louis Valatx, military doctor and researcher at INSERM (French National Institute of Health and Medical Research), It is not uncommon to observe repeated infarct lesions in nuclear test veterans, while they had no family genetic predisposition and that they had undergone the mandatory medical tests to be soldiers.
In his epidemiological survey of French military nuclear veterans, Jean-Louis Valatx was the only one to report that there are a multitude of pathologies other than cancers.
Current studies in the United Kingdom and France are intended to examine genetic mutation factors and trans-generational consequences, may determine genes involved in specific cardiac lesions.
Thus, if we demonstrate these phenomena to the competent authorities, prevention and follow-up will undoubtedly be possible and recommended, not only for nuclear test veterans but for civil nuclear workers, indigenous peoples and all the offspring of affected populations.
Bibliography
“AVEN Health Survey” (AVEN = French Nuclear Test Veterans Association). Accessed on 4th November 2018. http://www.aven.org/aven-acceuil-actions-medicales-enquete-sante
« Les rayonnements en médecine – Regards sur l’histoire de l’imagerie médicale – Dossiers – S’inspirer – Chercher, trouver – Bibliothèque – Lieux ressources – Au programme – Accueil – Expositions, conférences, cinémas, activités culturelles et sorties touristiques pour les enfants, les parents, les familles – Paris ». Accessed on 2nd November 2018.
http://www.cite-sciences.fr/
Accessed on 4
Nabiałek-Trojanowska, Izabela, Ewa Lewicka, Anna Wrona, Anna M. Kaleta, Zuzanna Lewicka-Potocka, Grzegorz Raczak, et Rafał Dziadziuszko. « Cardiovascular Complications after Radiotherapy ». Cardiology Journal 0 (16 October 2018). https://doi.org/10.5603/CJ.a2018.0120
« Maladies cardiovasculaires liées aux rayonnements: manifestations et gestion – ScienceDirect ». Accessed on 4th November 2018.
https://www.sciencedirect.com/science/article/pii/S1053429603000262?via%3Dihub
Spetz, Johan, Javid Moslehi, et Kristopher Sarosiek. « Radiation-Induced Cardiovascular Toxicity: Mechanisms,
Prevention, and Treatment ». Current Treatment Options in Cardiovascular Medicine 20, no 4 (20 March 2018): 31. https://doi.org/10.1007/s11936-018-0627-x
Liang, Xinyue, Shirong Zheng, Jiuwei Cui, Dehai Yu, Guozi Yang, Lei Zhou, Brain Wang, Lu Cai, et Wei Li. « Alterations of MicroRNA Expression in the Liver, Heart, and Testis of Mice Upon Exposure to Repeated Low-Dose Radiation ». Dose-Response: A Publication of International Hormesis Society 16, no 3 (September 2018): 1559325818799561.
https://doi.org/10.1177/1559325818799561
Kelly, R. G., and E. Buckingham. « The regionalization of cardiac gene expression: implications for heart morphogenesis. » M / S.
https://doi.org/10.4267/10608/908
